 
Targeted temperature management between 32-36 oC for comatose patients with ROSC for at least 24 hours is recommended. Low end tidal CO 2 (less than 10 mm Hg) after 20 minutes is associated with low likelihood of survival.ĮCMO or ECPR can be considered in patients with refractory cardiac arrest who have not responded to conventional CPR, where it can be rapidly implemented with suspicion of reversible cause of cardiac arrest.Įmergency percutaneous coronary intervention is recommended for patients with ST elevation on ECG and for hemodynamically or electrically unstable patients with no ST elevation but suspected cardiovascular cause. Provide 100% FiO 2 during cardiac arrest, with oxygen saturation titrated to greater than 94% post ROSC.Įnd tidal CO 2 can be used to monitor for ROSC. Steroids may provide some benefit when bundled with vasopressin and epinephrine in in-hospital cardiac arrest, though routine use is not recommended. Routine use of beta blockers after cardiac arrest is not recommended, with benefits for ROSC only demonstrated through animal studies and case reports. Vasopressin has been removed from the ACLS algorithm. If adjunctive or definitive airway is in place, provide 10 breaths per minute.Įarly defibrillation is the most effective modality for return of spontaneous circulation (ROSC).Īmiodarone or lignocaine (lidocaine) may not provide added benefit to defibrillation. 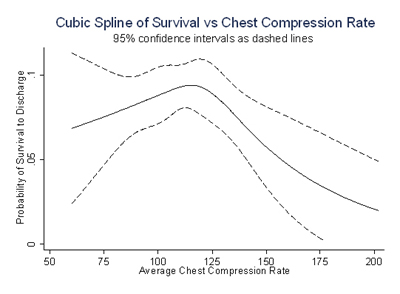
There does not appear to be an advantage to asynchronous or interpolated breaths as long as the highest possible compression ratio is maintained. Chest compression ratio should be > 60 and as close to 90 as possible. The recommended chest compression rate is 100-120 per minute, updated from 100 per minute.Ĭhest compression depth should be 5-6 cm, not more than 6 cm. Recommendations of the November 2015 AHA-ACLS updates 1 are provided in this chapter and are augmented by the most current resuscitation research literature. Cardiac resuscitation is a rapidly changing clinical science. 
0 Comments
Leave a Reply. |

 RSS Feed
RSS Feed
